In this article, we look at:

To stay happy and healthy, don't forget your 'intimate' flora!
The 10 best rated probiotics for women
Lactobacillus rhamnosus GR-1® - vaginal health
Lactobacillus reuteri RC-14® - vaginal health
Lactobacillus paracasei F-19® - vaginal health
Lactobacillus rhamnosus HN001 - vaginal health
Lactobacillus crispatus - vaginal health
Lactobacillus acidophilus NCFM® - bloating and IBS
Bifidobacterium lactis BB-12® - constipation and regularity
Bacillus coagulans Unique IS-2 - IBS
Lactobacillus rhamnosus HN001 - pregnancy
Bifidobacterium lactis HN019 - pregnancy
These are the best rated probiotics for women used by the most trusted and recommended expert probiotic brands in the UK.
How can probiotics help women?
Probiotics are live micro-organisms which offer health benefits to their host. The importance of supporting gut health with probiotics is becoming more widely recognised, but we don't just have a microbiome in our gut, we have them, all over the body, including our mouth, on the skin, in the lungs, and in the vagina. Therefore probiotics are not just used to support a healthy gut, they can be used to support overall health and wellbeing, and a variety of different health concerns, such as:
Follow the links to read in-depth articles on the Probiotics Learning Lab about these various aspects of health, or read on to explore in more detail which probiotics are best for women. Find out which strains are for vaginal health in the next section, or learn about the best probiotics for common female health conditions such as pregnancy, bloating and constipation.
Which are the best probiotics for women's vaginal health?
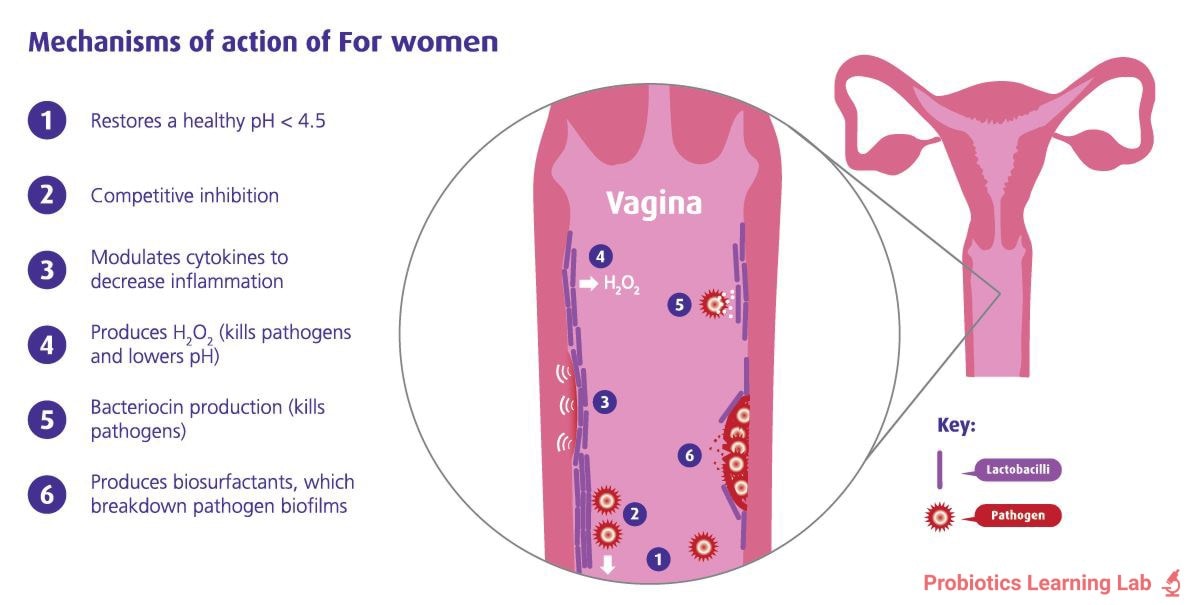
We often get asked what are vaginal probiotics? How are probiotics good for vaginal health? What is the best women’s probiotic for BV and/or thrush? To answer these questions, we first need to think about the anatomy of the intimate area, and how the vaginal microbiome may become unbalanced.
Typically, a healthy vaginal and urinary microbiome will be populated largely by Lactobacilli bacteria. These helpful microbes are thought to exert many of the same beneficial effects as they would in the gut: helping to maintain a healthy balance and discouraging bad bacteria or yeasts from overgrowing and causing conditions such as thrush, urinary tract infections (UTIs) and bacterial vaginosis (BV)1,4. However, due to the proximity of the vagina to the anus, it is much easier for bad bacteria and yeasts to translocate from the gut to the vagina to cause infections that it is for bacteria to cause health issues in the penis5.
It is believed that most infections like thrush, cystitis or UTIs stem from bad gut bacteria which have travelled through the digestive tract to the anus, across the perineum and over to the urogenital tract. Thankfully, good bacteria can take the same route! Not all probiotic strains will travel to the vagina, however, so if you are choosing a supplement, make sure it contains specific probiotics for vaginal health. Certain strains such as Lactobacillus rhamnosus GR-1® and Lactobacillus reuteri RC-14® have been shown to reach the vagina alive and colonise there, positively affecting the environment. Strains with these abilities are the best vaginal probiotics.
Another common question is "Can you put probiotics into your vagina?" The simple answer to this is "Yes", it's not unsafe to do so; however, probiotics were taken orally in most supporting research studies, so with an oral probiotic supplement containing strains proven to reach the vagina alive, you don't need to. According to the scientists who conducted one study, "L. rhamnosus GR-1® and L. reuteri RC-14® can translocate to the vaginal environment even if they are taken orally" and "Their administration results in significant changes in the vaginal flora in terms of increased Lactobacilli presence…"6.
This means that there is no need to put probiotics directly into the vagina, and they can be taken easily and more conveniently orally.
Healthcare professionals can learn more about the research behind Lactobacillus rhamnosus GR-1® and Lactobacillus reuteri RC-14® on the Probiotics Database.
Read on to find out more about the best probiotics for vaginal health and common vaginal infections.
Bacterial vaginosis
As bacterial vaginosis (BV) is the most common type of vaginal infection in premenopausal women7, finding a safe and natural approach to treatment/prevention would be a huge win. One significant study, a gold-standard randomised, placebo-controlled trial8 showed that the vaginal microflora in women with BV was restored to a more favourable, Lactobacilli-dominant environment following two months of taking the probiotics Lactobacillus rhamnosus GR-1® and Lactobacillus reuteri RC-14®.
During pregnancy, women often suffer from intimate health infections due to the hormonal changes taking place during this time. It is important for both the health of mother and baby that an expectant mother has a healthy vaginal microbiome, as during a normal vaginal delivery the mother passes on some of her resident microflora to her newborn. This transference of bacteria from mother to baby influences the health of the baby’s microbiome.
In 2018 a clinical trial9 showed that the probiotic strain Lactobacillus rhamnosus HN001 (in conjunction with Lactobacillus acidophilus La-14® and lactoferrin) is able to help reduce symptoms of BV, such as itching and discharge.
A clinical trial using Lactobacillus paracasei F-19® demonstrated the ability to improve vaginal pH and odour in those with vaginosis10, maintaining relief even 3 months after the end of treatment when taken orally.
A hig-quality probiotic designed to support BV might contain these strains, as they are some of the most well-researched for this condition.
Anyone with a vagina can develop BV, even those undergoing masculinising hormone therapy11, so it's important to always keep an eye on vaginal health.
Urinary tract infections
Urinary tract infections (UTIs) unfortunately affect people of all ages. It seems that in the genitourinary area of those who do not experience infections, Lactobacilli bacteria dominate1. The probiotic strains; Lactobacillus rhamnosus GR-1®, Lactobacillus reuteri RC-14®12 and Lactobacillus crispatus13 have been reported to support a healthy urinary microbiome in those who experience recurrent UTIs.
Healthcare professionals can learn more around this subject by reading the following articles on the Probiotic Professionals site:
Probiotics for UTIs - a look at the research
Thrush
Thrush is a very common vaginal complaint. It can occur due to vaginal imbalances caused by hormonal fluctuations at certain points in the menstrual cycle, during pregnancy and when taking the combined oral contraceptive pill or HRT (hormonal replacement therapy). When oestrogen levels are high, Candida, the yeast responsible for thrush, thrives14. A probiotic supplement that contains the well-researched Lactobacillus rhamnosus GR-1® and Lactobacillus reuteri RC-14® strains may help those prone to thrush, as they may help inhibit the growth of harmful bacteria and yeasts, such as Candida, in the vagina15. It can also occur when the vaginal microbiome is disrupted due to taking antibiotic medications - read more about taking probiotics alongside antibiotics.
A 2015 study16 looked at 40 women with recurrent vulvovaginal candidiasis (thrush), some were given the probiotic strains Lactobacillus rhamnosus DSM 14870 and Lactobacillus gasseri DSM 14869 alongside conventional treatment. The results showed that probiotics taken alongside conventional treatment increased the efficacy and reduced the risk of the infection coming back compared to conventional treatment alone.
Healthcare professionals can learn more by reading Which probiotics help with thrush? and Which Probiotics are best for Candida? on the Probiotic Professionals site.
Fertility
Vaginal infections including BV, UTIs and Group B Streptococcus (GBS) have been linked to complications in pregnancy and even reducing the chance of getting pregnant in the first place17. It can be an important consideration for any pre-conceptual regime to incorporate a probiotic that addresses the vaginal microbiome, especially if the infections are reoccurring.
The beauty of these specific probiotics is that not only do they reduce symptoms, but they also appear to act against recurrence. For the 1 in 3 people with vaginas who suffer from BV, 30% who suffer recurring cystitis and 75% who suffer thrush at least once, these strains of probiotics could be a welcome addition to their tool kit to rid themselves of these uncomfortable conditions.
Can probiotics make your vagina smell better?
A few years back there was some buzz around a probiotic supplement that claimed to get your vagina smelling like a peach! However, this turned out to be misleading and was not intended to change the smell of the vagina; as far as we know there aren’t any probiotics that can produce a fruity aroma in the vagina!
However, it’s true that when you have a vaginal infection, the smell (e.g. in the case of bacterial vaginosis) can be unpleasant and upsetting. Probiotics can indeed help to solve this problem and get you smelling fresh, naturally!25
Which are the best probiotics for women's digestive health?
The vaginal flora is supported by different probiotic strains to those recommended for gut health. Whilst probiotic strains for digestive health conditions are not typically gender-specific, there are a few digestive symptoms which are commonly experienced by women. Women tend to have a slightly longer colon than men, meaning that stool transit time can be longer and women are more likely than men to suffer from IBS-type symptoms such as constipation and bloating2. Other factors, such as pregnancy, menstruation, and other hormonal influences along with differences in lifestyle can also lead to a higher incidence of digestive issues in women3. Let's explore which probiotic strains have been researched for these conditions:
Bloating
Bloating is an extremely common concern. This may be a constant problem, or the bloating may be cyclical and worsen at certain times of the menstrual cycle (e.g. premenstrual bloating) or around menopause.
There are several factors that can lead to bloating, characterised by a swollen, uncomfortable abdomen. Fluctuating hormone levels, stress, poor diet or disturbed digestion (IBS, food intolerances for example), to name a few. Upset digestion associated with menstruation is very common, including alterations to bowel patterns, constipation, diarrhoea, nausea, abdominal pain and bloating18. Fluctuating levels of female sex hormones, oestrogen and progesterone, and the body’s sensitivity to these fluctuations is thought to contribute to the sensation of bloating that occurs around menstruation19. Research shows that certain probiotic strains may help to alleviate this bloating and digestive discomfort, such as Lactobacillus acidophilus NCFM®.
Additionally, the probiotic strain Bacillus coagulans Unique IS-2 was shown in a gold-standard clinical trial to reduce symptoms of IBS in adults20. From week five the probiotic group exhibited significant improvements in abdominal discomfort, bloating, urgency, incomplete evacuation, straining, passage of gas and bowel habit satisfaction.
Bacillus coagulans Unique IS-2 is part of a group of bacteria known as soil-based organisms which are commonly used in food, beverage and gummy supplement production due to the robust nature of this bacteria.
Health professionals can read more about Lactobacillus acidophilus NCFM® and Bacillus coagulans Unique IS-2 on the Probiotics Database.
You may like to read the following article: Bloating – all you need to know to learn more about bloating.

Bloating is a common issue that can cause considerable discomfort
Many women experience a bloated stomach in menopause that might be relieved with a few simple measures to look after their gut health, and the health of the microbiome. However, persistent bloating should never be overlooked and should be investigated by a GP, as persistent bloating can be signs of more serious conditions.
Constipation
As previously mentioned, constipation is more frequently reported in women than men21, often occurring around menstruation, during pregnancy and post-menopause. A probiotic supplement containing Bifidobacterium lactis BB-12® can help support gut health in those with constipation. B. lactis BB-12®, along with fructooligosaccharides (FOS), a type of prebiotic, can help gently encourage regular bowel movements, as supported by one of the largest clinical trials performed on probiotics22. This strain of probiotic is often used by women with regularity issues.
Health professionals can read more about the research behind this strain on the Probiotics Database: Bifidobacterium lactis BB-12®.
Alterations to normal bowel patterns, including constipation, can also occur as a part of IBS (Irritable Bowel Syndrome). Symptoms of IBS, including abdominal discomfort and disrupted bowel patterns, can be exacerbated around the time of menstruation in those with menstrual cycles and in perimenopausal women23.
To learn more about how to support gut health in IBS, read Which probiotics are for IBS?
For more information about supporting clients with occasional constipation, healthcare professionals can read Probiotics for Constipation on the Probiotic Professionals site.
Pregnancy
Some strains of probiotics such as Lactobacillus rhamnosus HN001, Lactobacillus acidophilus La-14®, and Bifidobacterium lactis HN019, have been researched specifically in pregnancy and found to support common pregnancy-related concerns such as digestive issues, morning sickness, gestational diabetes, and mental wellbeing.
For everything you need to know about using probiotics at this special time, read Probiotics for Pregnancy.
Which is the best probiotic for women?
It can be confusing to know how to choose the right probiotic for women, as there are many different types of probiotic supplements available, including capsules, liquids and powders. Most women tend to prefer a capsule as these are easy to fit into a morning routine. For women who don’t like taking capsules or powders, then gummy products for adults are now available. However, it is important to select gummies which contain very robust strains of bacteria (known as soil-based organisms) which allows them to survive the manufacturing process, for example Bacillus coagulans Unique IS-2.
It's good to look for the most recommended probiotics, so check out the reviews for your chosen brand. But the most effective probiotic for women will be the one which is most suitable for their individual needs. Therefore if you are seeking specific health benefits, such as the best probiotic for women over 50, consider a friendly bacteria supplement with research supporting its use for this particular purpose. For example, if you are looking for probiotics for vaginal health, consider a product that contains well-researched strains including L. paracasei F-19® and the world-renowned L. rhamnosus GR-1® and L. reuteri RC-14® which have shown to help support a healthy vaginal microbiome24.
If you’re confused as to what ‘well-researched’ really means, what is meant by terms such as 'billions CFU', or why research is so important, you might like to read this helpful article: Research: is it all equal?.
If you’ve never taken probiotics before and are wondering if they’d suit you, then be reassured that the potential benefits of probiotics are numerous, but any side effects are rare, making these supplements a popular choice for daily maintenance of gut and intimate health.
Healthcare professionals can reassure their clients about this topic by reading Probiotics and side effects – an in-depth review on the Probiotic Professionals site.
Should women take probiotics every day?
With a very few exceptions, it is safe - and generally advisable - for women to take probiotics every day. Read more about using probiotics daily in this article: Can I take probiotics every day? If you have serious health conditions or are taking medication, then speak to your doctor before taking any natural supplement.
Key take-aways:
Probiotic supplements are not usually gender-specific, but certain strains have been researched specifically for the support of female health issues such as vaginal infections, and pregnancy.
Probiotics can help to limit the overgrowth of harmful bacteria and yeasts that contribute to the development of gut and intimate health issues.
Women often suffer from digestive issues, such as constipation and bloating, more often than men.
The vagina and urinary tract require different friendly bacteria to the gut to maintain a healthy microbiome.
Look for specific probiotic strains which have been researched for your individual needs.
For more information about other supplements for women’s health, read Kathy’s article: Supplements for women: which do you really need?
You may also be interested to read the following related articles: