First of all, to make it through the digestive tract, live cultures need to be a high-quality robust strain, otherwise their journey will be over before it’s begun!
In a high-quality probiotic supplement, the strains will have the following features:
Survive stomach acidity
Reach the gut alive
Inhibit the growth of pathogens (harmful microbes)
Let’s look at each stage in more detail.
When to take probiotics
To start their journey through the digestive tract, probiotic bacteria need to be able to survive the stomach environment. Even robust strains will find this a challenge, so to give them the best chance of survival probiotic supplements are best taken in the morning with, or just after, breakfast. The reason for this is that the acid in our stomach is at its lowest level in the morning1, and this acidity is buffered still further by the presence of food in the stomach. Stomach acid is an important defence against pathogens as it helps to kill harmful bacteria as they enter the stomach in our food and water. In this way, it helps to prevent foodborne disease and is very useful. However, in a similar manner, it can also damage certain probiotics as they pass through the stomach to the gut2.

How do probiotics survive stomach acid to arrive in the gut?
So, to sum up, we can see that timing can be a key factor to ensure the survival of probiotics through the harsh stomach environment. By taking a probiotic supplement in the morning with breakfast you can ensure that the bacteria travel safely through the acidic stomach environment and arrive at their destination in the gut. It is important to select robust strains of bacteria that are naturally resilient to acidic conditions and have been tested to ensure their viability at different acid levels3. To learn more, read Do probiotics survive stomach acid?
How do probiotics work in the gut
Once through the stomach, the probiotic bacteria embark on the next stage of their journey. They are released into the small intestines, where some strains will begin to take up ‘residence’ for a short time. Other strains may pass through the small intestine and take up residence when they reach the large intestine (or bowel). Where probiotics choose to reside is governed predominantly by the specific conditions in different areas of the gut including pH (levels of acidity or alkalinity), oxygen levels, and the type of bacteria in the microbiome4.
Some areas of the gut have more oxygen available like the small intestine, whereas other areas have little or no oxygen like parts of the large intestine, making those areas only suitable for certain strains of bacteria that do not need oxygen to survive. Additionally, the pH differs at different points along the digestive tract, with the small intestine typically being more acidic than the large intestine. Although, as we have learned, it can be a challenge for probiotic bacteria to travel through the highly acidic stomach, which can reach acidity levels of around pH 1.5, probiotic bacteria actually prefer a slightly acidic or pH neutral environment5. All these factors influence where particular strains of bacteria choose to ‘live’.
To assess if a probiotic strain has the ability to reach the gut alive, specific laboratory tests are undertaken to detect the presence of the probiotic strain in the individual’s stool after supplementation6,7,8. It is important to choose a probiotic supplement which contains strains that have been proven to reach the gut alive. It is commonly believed that probiotics need to be taken in enteric-coated capsules to protect the probiotics as they pass through the stomach before being released into the gut. This is not necessary for probiotic strains which are resilient and able to reach the gut without damage. Learn more about common probiotic myths by reading The Survival Myth.
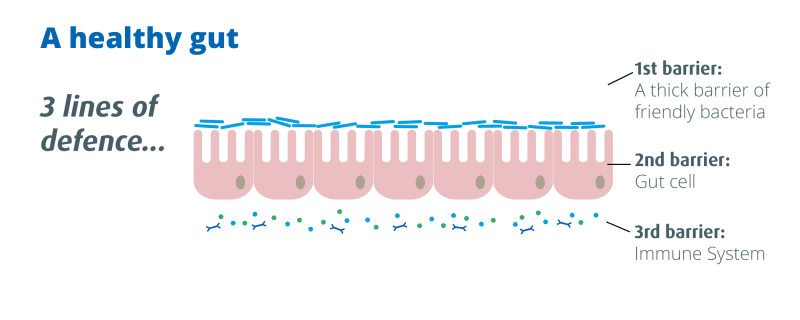
What do probiotics do?
By rapidly growing in numbers, probiotics can ‘crowd out’ any pathogenic (or ‘bad’) strains of bacteria that may have been able to take hold. The good bacteria compete with pathogens for both their food sources and space in which to live, making it difficult for the undesirable bacteria to survive9. Probiotics also work by producing certain acids10 which discourage pathogen growth, whilst improving the gut environment for their own benefit and for the benefit of other types of good bacteria, which also begin to grow in numbers.
When the gut microbiome comes into balance with increased levels of beneficial bacteria and reduced levels of pathogenic bacteria, the individual may notice an improvement in their digestion and wellbeing. This is because gut pathogens produce many toxins11 and other substances that negatively affect our health, whereas probiotic strains of bacteria produce beneficial substances, including certain vitamins and short-chain-fatty-acids that have a positive impact on our overall health.
Our gut is home to a delicate ecosystem of microbes, and many factors affect which strains flourish, and which ones may struggle. When we take a probiotic supplement, not only are we introducing new friendly bacteria to the gut, we are also facilitating the growth of our own indigenous friendly bacteria. Probiotics impact our gut health in such a way that our own natural resident strains of ‘friendly’ bacteria can recover and replenish8.
How long do probiotics take to work?
The time it takes for probiotics to work depends on the probiotic strain being used, the composition of the gut microbiome of the individual and the symptoms the individual is experiencing. Everyone is unique with different gut microbiomes, each as unique as our fingerprints12. Therefore, it can be difficult to predict how quickly an individual will respond to a particular probiotic supplement.
When it comes to specific probiotic strains, each strain has a different effect on the gut microbiome. For example, significant improvements in a range of digestive symptoms were seen within 2 weeks when Bifidobacterium lactis HN019 was supplemented daily13. Other strains such as Lactobacillus reuteri RC-14® and Lactobacillus rhamnosus GR-1® when taken daily have been detected in the vaginal flora 7 days14 after starting probiotic supplementation. However, improvement of symptoms when taking these strains was noted after a month of supplementation15. In contrast to this, Saccharomyces boulardii, the probiotic yeast, has been shown to have beneficial effects quite quickly, notably in one trial, within 3 days16. Find out more on this topic by reading Are all probiotics the same?
As a result, it can be difficult to pinpoint exactly when the effects of a specific probiotic supplement will be noticed. It is always a good idea when starting a new supplement to keep a journal of symptoms you are experiencing from before you start the supplement and for the first few weeks of taking it. This will help you to keep track of any changes you notice to your health as you introduce a new supplement and be alert to the signs probiotics are working. Keep in mind that your body will have a unique response to probiotic supplementation which is dependent on factors specific to the individual.
How to tell when probiotics are working

You may find the following article of interest to increase your understanding of how do probiotics work: Benefits of Probiotics
Good health starts in the gut, and it’s best to address any presenting digestive symptoms regardless of which health condition you’re trying to support. If people are generally well or have good digestion, they may not initially notice a drastic change when they take a probiotic supplement. But so many different things can affect the gut microbiome, such as medications, stress, and poor diet, that it’s always good to keep the gut microbiome well supported by taking probiotics and eating fermented foods. Also, over a longer period of time they may notice positive changes, such as less frequent colds or skin breakouts. For others, when they are taking a probiotic supplement for a specific condition, they may notice a specific improvement in that area. However, having a healthy microbiome is just one consideration when supporting any health condition; for a fully holistic protocol a doctor should be consulted, and a health professional such as a nutritional therapist, who can also advise on diet and lifestyle.
Summary of how probiotics work
A probiotic can only work if it is capable of surviving the harsh stomach environment. If you have selected a strain that is proven to reach the gut alive help it out by taking it in the morning with your breakfast.
The probiotic will take up short term residence in either the small or lage intestine depending on the conditions in these areas.
Once in situ the probiotics can ‘crowd out’ any ‘bad’ bacteria by competing for their food sources and space.
Probiotics will also provide certain vitamins and short chain fatty acids which are known to be beneficial for our health.
Depending on the specific strain chosen changes to the gut can be noted from as little as 3 days.
You should now feel confident that you have the knowledge to answer the following commonly asked questions:
If you found this article interesting, you may also like to read:









