Could we have found a way to naturally support those with atopic dermatitis, more commonly known as eczema?
Within this article:
Atopic Dermatitis manifests itself as dry and scaly skin which is intensely itchy and can develop into sore cracked skin
What is Atopic Dermatitis?
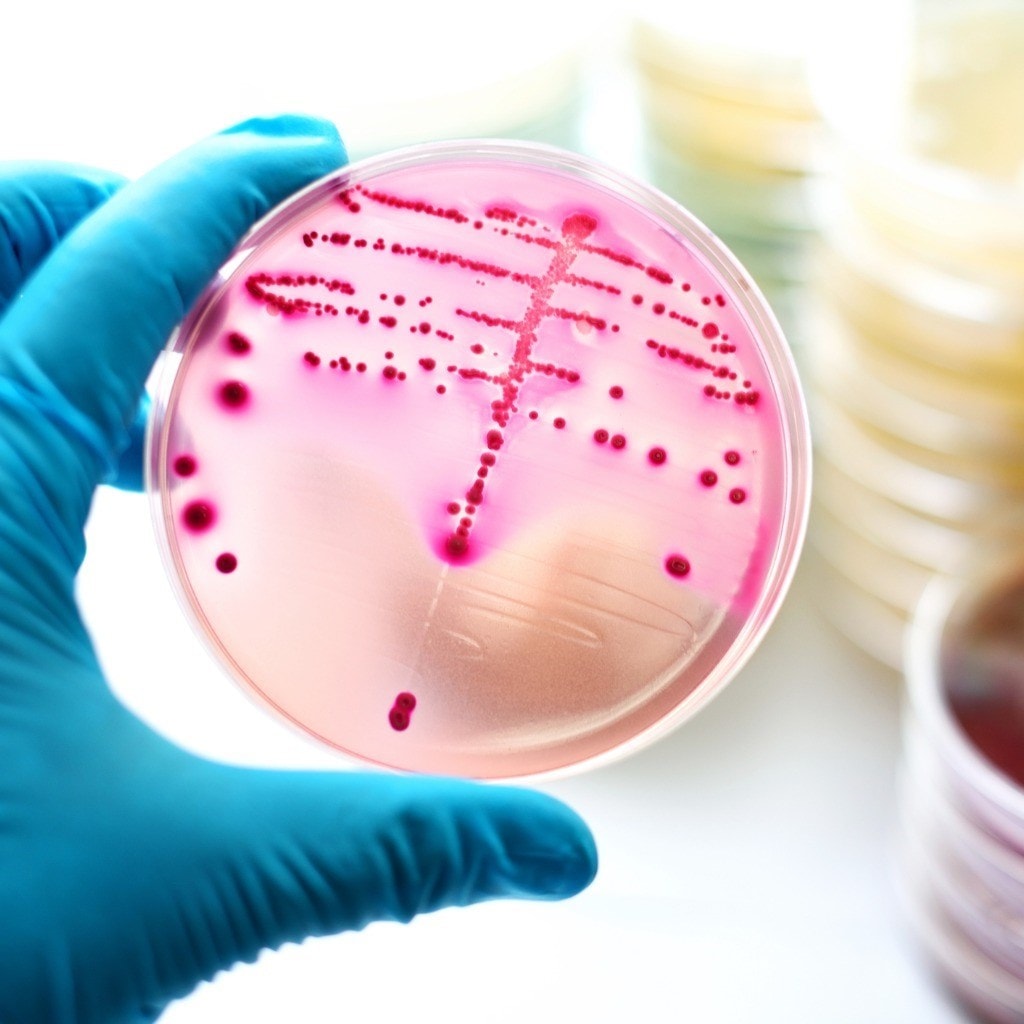
Atopic Dermatitis affects many children and although many grow out of it, it can persist into adulthood. It manifests itself as dry and scaly skin which is intensely itchy and can develop into very sore cracked skin. It’s a debilitating and distressing condition and it’s not really known what causes it. Genetics and an impaired diversity of gut bacteria are among the causes researched. A large part of the problem is to do with impaired skin barrier. A protein called filaggrin which is an important component of the skin barrier can sometimes be lacking due to a genetic mutation. As well as this it has been found that atopic dematology patients with Staphyloccous aureus biofilms (MRSA and MSSA) present are much harder to treat and result in a more severe condition. These biofilms are caused by bacteria that block sweat ducts and cover the skin causing an immune response and therefore itching. A recent study shows that there appears to be more than one way in which live cultures can help alleviate this condition.
The Study
We already know that live cultures can help reduce eczema by reducing intestinal inflammation, therefore promoting endogenous barrier mechanisms, and ultimately alleviating the eczema. We are therefore used to talking about how live cultures in capsule form can help combat eczema. However, this study1 suggests that live cultures can also be used topically when treating eczema. The study which is lead by Eva Berkes, MD, chief scientific officer for Quorum Innovations in Sarasota in Florida found that a live culture extract could offer drug-free topical therapy for patients with atopic dermatitis as well as protecting against pathogenic biofilms.
The researchers took a live culture extract developed from a human microbiome. The good bacteria was ‘physically processed’, without chemicals, to increase its activity so it works more intensely than in its pure form. In this study the extract was then used on normal skin samples taken from plastic surgery patients.

Topical steroids can only give temporary relief
Two different tests were made. In the first one a detergent was used to remove the natural lipid layer on the skin and dry it out to resemble atopic dermatitis. The topical live culture extract was then applied to this skin and they found that the effect was similar to the steroid normally used in that the extract restored the integrity of the skin barrier. As well as this, it was found that this treatment increased the levels of filaggrin protein (which is an important component of skin barrier) twofold compared to the untreated skin.
In the second study, the live culture extract treatment was tested for three anti-biofilm properties: adhesion, inhibition and detachment. It was found that the anti-adhesion properties doubled compared with skin treated by antibiotics. The extract was as effective as the antibiotics in inhibiting a MRSA biofilm. And finally five times more effective at detaching MRSA biofilm. Not only this but this extract bioactively inhibited 50-60% of MSSA biofilm formation.
As Dr Berke explained, this last point is of huge potential benefit as biofilms are the cause of almost all hospital acquired infections. "All antibiotics approved by the FDA to date have been tested only in the free-floating form, not attached to any surface," she explained. "However, both pathogenic and benign microbes that live on body surfaces preferentially live in biofilm form. They live in communities protected by microbially-produced extracellular polymers that confer tremendous defence against antibiotics." With current antibiotics being “notoriously bad” at killing pathogenic biofilms, “this is an area of tremendous need,” said Dr Berkes”
Read more on how live cultures could help reduce hospital infections.
Why not steroids?
Topical steroids of varying strengths are used on the skin. They can give temporary relief but it must not be forgotten that these are absorbed into the structure of the skin and then further into the body so invariably will have an effect beyond the relief desired.
Undesirable side effects when used long term include thinning of the skin, easy bruising, enlarged blood vessels, and susceptibility to skin infections and aggravation of certain skin conditions. As well as this they can suppress the adrenal gland, resulting in the body not producing its natural steroids so stopping steroids suddenly can then result in illness. Additionally large amounts absorbed through the skin can cause fluid retention, raised blood pressure and diabetes among other things. It would therefore follow that steroids need to be used with a little caution and a natural alternative would be welcome
Eczema has increased by 40% over the last four years in the UK alone. It can affect 10% of children and although many go on to grow out of it, many also continue to suffer from this into adulthood. To find a solution that would be natural, safe and effective, yet with no side effects would be a real result and help thousands of people. We look forward to reading any further research into the topical effects of live cultures.
You may also like to read our article on probiotics and eczema which covers the latest research on specific strains shown to reduce the severity of eczema.